BioElectronics Clinical Studies: Chronic Musculoskeletal Pain
Pulsed electromagnetic fields in knee osteoarthritis: a double blind, placebo-controlled, randomized clinical trial
 This trial aimed to test the effectiveness of a wearable pulsed electromagnetic fields (PEMF) device in the management of pain in knee OA patients. This study was published on December 24, 2015 by Rheumatology (Oxford).
This trial aimed to test the effectiveness of a wearable pulsed electromagnetic fields (PEMF) device in the management of pain in knee OA patients. This study was published on December 24, 2015 by Rheumatology (Oxford).
RESULTS:
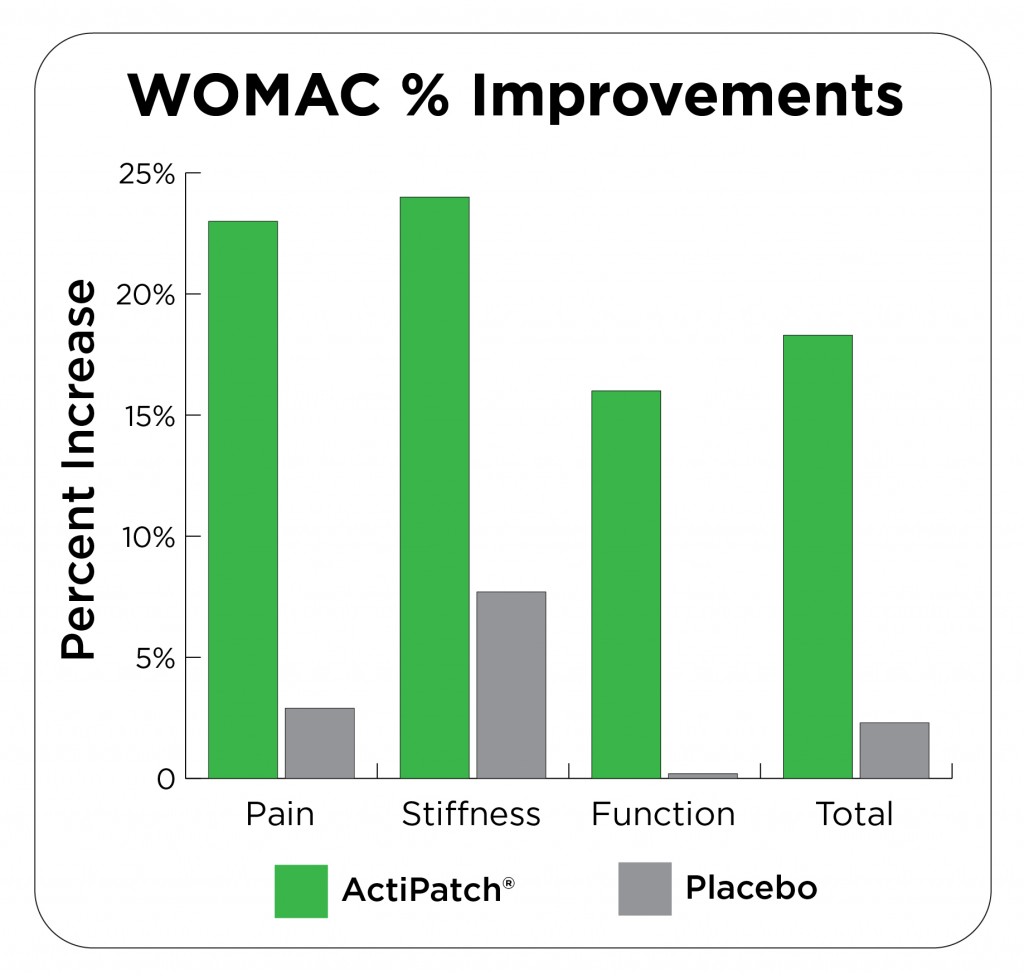
Sixty-six patients were included, and 60 completed the study. After 1 month, PEMF induced a significant reduction in VAS pain and WOMAC (Western Ontario and McMaster Universities Osteoarthritis Index) scores compared with placebo. Additionally, pain tolerance, as expressed by PPT changes, and physical health improved in PEMF-treated patients. A mean treatment effect of -0.73 (95% CI – 1.24 to – 0.19) was seen in VAS score, while the effect size was -0.34 (95% CI – 0.85 to 0.17) for WOMAC score. Twenty-six per cent of patients in the PEMF group stopped NSAID/analgesic therapy. No adverse events were detected.
CONCLUSION:
These results suggest that PEMF therapy is effective for pain management in knee OA patients and also affects pain threshold and physical functioning.
Click here to view the published study
BioElectronics’ Landmark 5,000+ Chronic Pain Patient Study Published in Pain Management Medical Journal
 Musculoskeletal pain is wide spread in society, negatively impacts quality of life and is currently inadequately treated for most people. BioElectronics Corporation (the manufacturer of ActiPatch®) has conducted a 7-Day trial program in the United Kingdom and Ireland. The reported responses indicate that it is an effective pain therapy for a wide range of common conditions causing pain including osteoarthritis, rheumatoid arthritis and fibromyalgia.
Musculoskeletal pain is wide spread in society, negatively impacts quality of life and is currently inadequately treated for most people. BioElectronics Corporation (the manufacturer of ActiPatch®) has conducted a 7-Day trial program in the United Kingdom and Ireland. The reported responses indicate that it is an effective pain therapy for a wide range of common conditions causing pain including osteoarthritis, rheumatoid arthritis and fibromyalgia.
A registry study of 44,000 users of its ActiPatch 7-day trial device has been published in the prominent peer reviewed medical journal Pain Management. More than 5,000 chronic pain sufferers responded to the survey and submitted an assessment. Click here to view the article
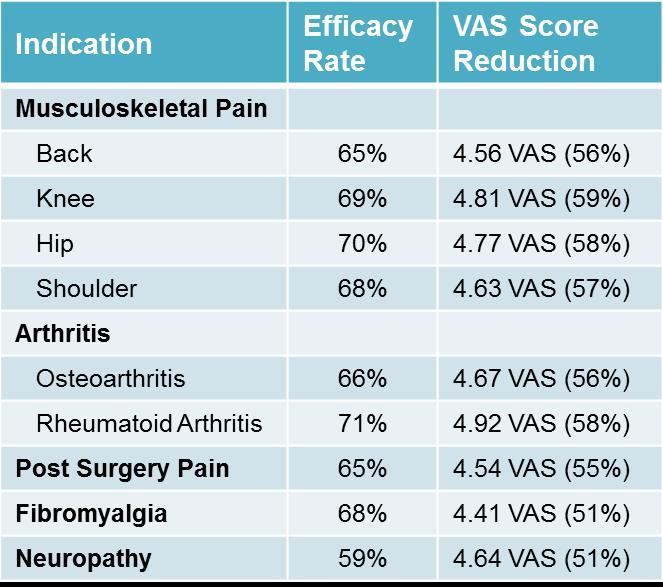
Chronic pain is a major unmet medical need that affects 20 to 40 % of the global population (more than diabetes, heart disease and cancer combined.) The majority of chronic pain causes, 80-85%, are musculoskeletal in nature. Despite using an average of 1.9 drugs for pain, 86% of the respondents reported that prior to using ActiPatch, they had pain levels of 8+ on a 11 point VAS scale- indicating severe unresolved pain. Pain was reduced an average of 57% for 65% of ActiPatch Therapy users who reported suffering from conditions such as osteoarthritis, rheumatoid arthritis, fibromyalgia, sports injuries, post-surgical pain, tendonitis, and neuropathy. There were no side effects reported.
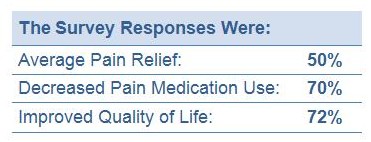
A 3-month follow-up analysis indicated 80% of ActiPatch users continued to purchase and use ActiPatch. The long-term effectiveness of ActiPatch therapy was confirmed by 93% of survey respondents reporting sustained pain relief, a distinct decrease in their medication use, and a significant improvement in their quality of life.
Key user findings:
- Average 50% reduction in medication use, including prescription drugs
- 67% including opioid users reported moderate to complete elimination of pain medication
- 70% reported better sleep
- 74% reported they are more physically active
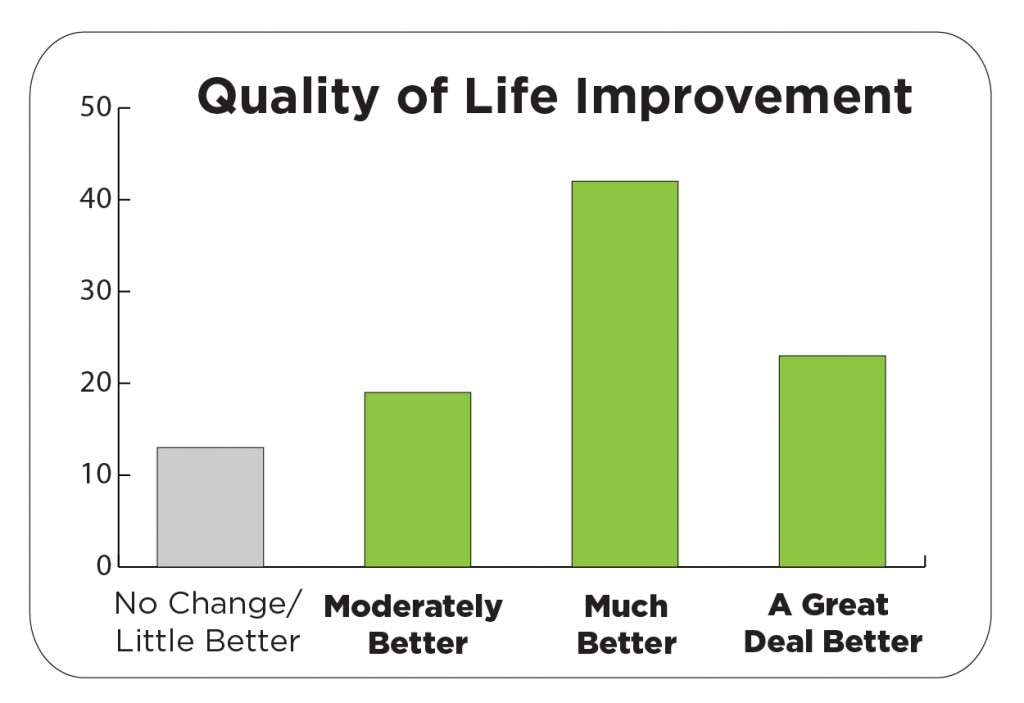
- 84% reported a moderate to a great deal better quality of life.
- 85% stated they would continue long term use of the retail device
Click here to view the published article
View Complete ActiPatch® Customer Survey
Plantar Fasciitis – Heel Pain
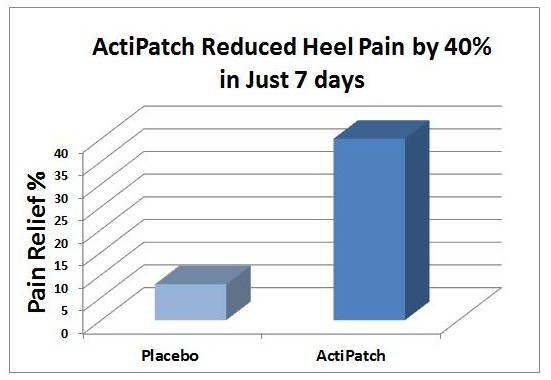
A multicenter, double blind, placebo controlled trial which showed that ActiPatch® as an overnight therapy was effective at rapidly reducing plantar fasciitis heel pain. The study is now published in the Journal of Foot and Ankle Surgery.
View Complete Plantar Fasciitis Heel Pain Clinical Study
ActiPatch Sleep Study: Chronic Pain and Sleep
A new hypothesis, which has attracted more and more attention, is that disturbances of sleep cause or modulate acute and chronic pain. Laboratory based sleep deprivation studies have also suggested that reductions in total sleep time are accompanied by increased sensitivity to noxious stimuli (secondary hyperalgesia) and by decrements in endogenous pain-inhibitory processes. This could also be a link between chronic pain and central sensitization (CS). In patients with osteoarthritis (OA), more than half experience pain during the night, resulting in sleep disruption, poor sleep quality, sleep fragmentation and frequent shifts between sleep stages. Recent studies have shown that sleep disruption can be a predictor of pain severity. Sleep disruption, therefore, could be associated with increased pain sensitivity and enhanced pain facilitation in addition to reduced pain inhibition in persons with chronic pain. Data has shown that severity of sleep disruption are associated with altered pain processing, and that sleep interventions for persons with knee OA-related pain might contribute to pain reductions.
In general people with insomnia and other sleep problems have increased sensitivity to pain. Sleep disruption appears to be associated with altered pain processing and central sensitization.
Conclusion
For those that have sleep interference due to their pain, decreasing their pain scores is closely related to sleep improvement.